Becoming a parent for the first time can be overwhelming. From sleep deprivation and navigating a whole new reality to learning to trust your instincts, it can be tough knowing whose advice to follow.
In this post, we’ll share the story of a new mom Torie and her son Myles, who faced significant challenges in their first year together. From antibiotic exposure at birth to never-ending reflux and fussiness, this research-savvy mom set off on a journey to find the root cause of her son’s relentless bouts of screaming.
During our chat with Torie, she inspired us with all the big and little sacrifices she made to figure out why Myles was in so much pain and discomfort. On the impossibly tough days, when doctors’ advice fell flat and her loved ones told her to accept that her son was just a fussy baby, she looked deeper. With her son’s health and happiness at stake, this first-time mom’s sleuthing skills eventually paid off.
We hope that reading Torie's story will bring you encouragement. You know your baby better than anyone. Advocating for your little one until you find answers that feel right in your bones takes moxie. And thanks to Torie, we get to see how it’s done.
A complicated start
Myles was born at 38 weeks after a quick 6-hour labor. Torie’s Group B Strep (GBS) test results weren’t in yet. Due to the rapid pace of the delivery, her doctors were only able to administer one dose of antibiotics, rather than the two doses typically given to prevent infection at birth. Torie’s OB/GYN decided to treat mom and baby as though they were positive for GBS and gave them both antibiotics.
Adding to those delivery room complications, Myles had trouble breathing. Doctors decided to treat them both with an additional dose of antibiotics, and Torie didn’t think much of it at the time, wrapped up in the whirlwind of her little one’s arrival.
Breastfeeding presented further challenges for Torie. “My milk didn't come in for a full week and Myles lost a bunch of weight,” she recalled. And even when her breastmilk production normalized, breastfeeding was painful and Myles had issues latching, a common breastfeeding problem. “It wasn't until he was eight weeks old that they found out he had a tongue and a lip tie,” Torie shared. Getting them corrected helped a little, but didn’t resolve Myles’ fussiness.
“He essentially screamed the first year of his life. It was a really long road.”
By his four-month pediatric visit, Myles was spitting up 40 to 50 times a day, so his pediatrician prescribed acid reflux medication. The treatment didn't reduce the frequency of Myles' spitting up but did help ease his pain. Torie had expected more. Feeling dismissed and frustrated to be told Myles’ fussiness was normal, she flexed her research skills and started exploring how her own diet might be triggering Myles' discomfort.
Myles remained on his acid reflux medication for two or three months while Torie began an elimination diet. She joined Facebook support groups, searching for advice from other moms, and pinpointed that dairy, spicy foods, anything cooked with oil, and acidic fruits like tomatoes upset Myles’ stomach. “I just had a very, very bland diet. I was determined, because I knew every time I ate something ‘bad’, he would be up all night screaming and crying,” Torie said. As difficult as it was to eat a restrictive diet, Torie was determined to ease her son’s pain.
“As a mother, you'll sacrifice anything for your child, do anything to keep them happy and healthy."
Her efforts made a subtle difference. “I figured out what worked and what didn't for two or three months. And then I stopped giving him the meds because I was controlling it, but he was still spitting up,” Torie said.
“I felt very isolated and alone”
Prolonged, intense crying—characteristics of colic in an otherwise healthy baby—can be incredibly discouraging for any parent, when no amount of consoling seems to bring relief. But colic typically resolves by a baby’s third or fourth month of life. By the time Myles was about seven months old, Torie was calling her pediatrician in tears most weeks and became close with the nurse on the after-hours hotline. "I would just cry to her, and she wanted to help so bad," Torie said.
The lack of sleep and constant worry took a toll. "I felt very isolated and alone with my struggles because no one understood what I was going through behind closed doors. I even took him to the ER one day when he wouldn't stop screaming. I couldn't calm him down… and they did nothing. We believed there had to be something we could do as parents."
When Myles was ten months old, Torie got mastitis—an inflammation of breast tissue that sometimes involves an infection—and had to supplement his diet with formula. Though she gave him a hypoallergenic formula, he had an adverse reaction, and became even sicker. “Everything came back with a vengeance, and I could not get it back under control,” she recalled.
Their pediatrician referred Torie to a GI specialist, who immediately recommended Myles’ go back on reflux medications and schedule an endoscopy, a procedure that would need to be done under sedation because of Myles’ age. They tested him for allergies, and everything came back normal.
Amid this rollercoaster, some good news. Torie became pregnant with her second child. Myles had been doing well for about a month, but then his symptoms worsened. “I thought, I can't have another baby with this still happening. So I went back to my research," Torie said.
Discovering Tiny Health: the power of personalized care
In her search for answers, Torie learned about the importance of gut health. She went to her local health store and picked up a baby probiotic. They tried it for about a month, with no success. But then came a turning point.
Torie discovered Tiny Health through an online search. Initially skeptical, she sat on the decision for a few days, but felt she had tried everything else and had nothing to lose. “I just decided that it was worth it for his health and happiness and my sanity,” she recalled.
So Torie ordered a Baby Gut Health Test, took Myles’ sample, and filled out the Tiny Health survey following his test. “I came to the question asking if he’d ever been on antibiotics, and I put no and moved on… later on, down the page it asked about labor or c-section and all of a sudden I realized, I DID have antibiotics and I completely forgot. That's when it all clicked for me, that his gut health was just so screwed up from day one,” Torie said.
Myles’ first Baby Gut Test results arrived just before his first birthday and revealed a striking imbalance: While beneficial bacteria made up 40% of his sample, he only had 3.37% Bifidobacterium, a key species that should dominate a little one’s gut in the first year of life, as it protects against unfriendly microbes and trains their immune system [1].
His follow-up test months later showed his Bifidobacterium levels had jumped to 27.6%, moving from the "needs support" range to "great results.”
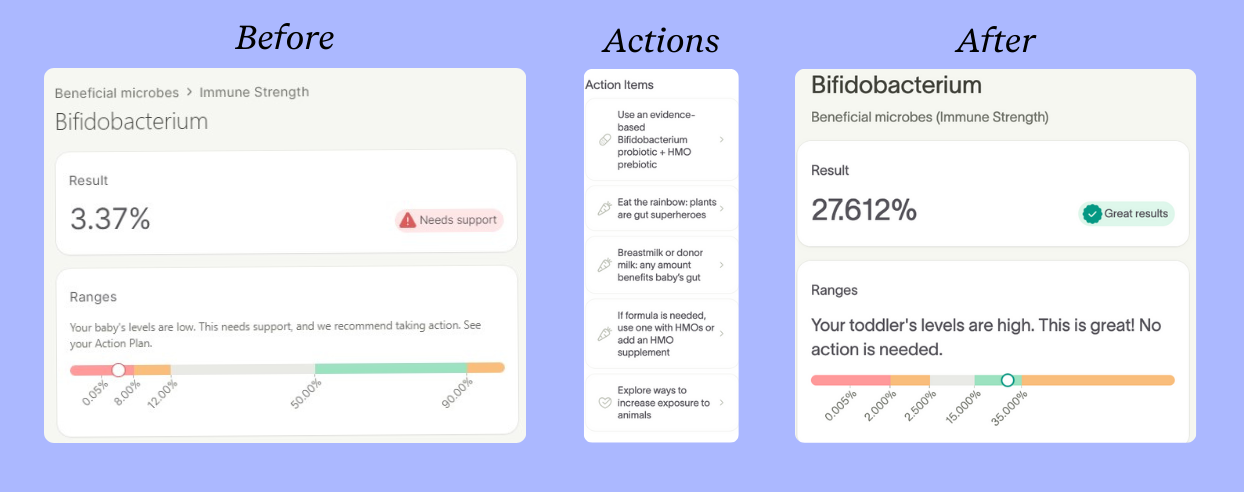
By following the Bifidobacterium probiotic recommendation in Myles’ Action Plan, Torie was able to bring his levels into the normal range. She also learned why the generic brand she picked for her son hadn’t made a difference—it didn’t contain the specific strains of beneficial bacteria he needed.
Myles also had an overabundance of Ruminococcus gnavus, a particular species of bacteria from the Lachnospiraceae family that is problematic at high levels in babies, because it has been associated with atopic march and allergic diseases [2], [3].

"It blew my mind how his good bacteria was almost extinct, and his bad bacteria were so far off the charts," Torie remembered. Myle’s resample results show how impactful his personalized recommendations (including adding more plant diversity and breast milk) were in course-correcting.
Another flagged metric in Myles’ Tiny Health report was a higher level of Escherichia flexneri, an unfriendly bacteria that is common in young children. These bacteria are generally fine at low levels, but can cause severe infection if left unchecked [4].
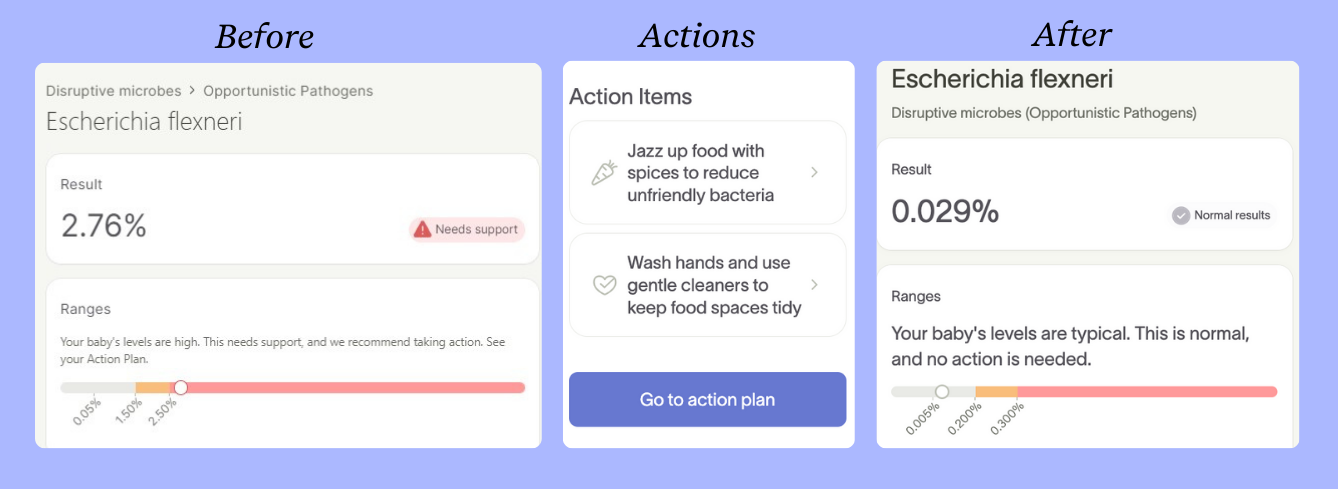
To reduce this unfriendly microbe, Torie used the spice chart in Myle’s Action Plan. “The specific spices the chart recommended were garlic, clove, and cinnamon and that was so easy. Oatmeal in the morning, sprinkle some cinnamon in it, Torie said. The initial results came in around Thanksgiving, so Torie made little pumpkin muffins for Myles with those added spices.
Torie was amazed that Myles showed improvements with just these simple dietary additions. "Then we got the probiotics, and at the two-and-a-half-week mark, I had a new kid," Torie said.
“I was just so impressed because it wasn't a gimmick. The fact that it talked about natural and free remedies like exposing him to different germs… it wasn't like, ‘here's the problem but give us more money to fix it.’”
All those changes paid off. Myles' most recent test showed his Microbiome Summary Score jumped 25 points, reflecting no major imbalances. (Tiny Health's Microbiome Summary Score evaluates all the relevant metrics for an age range into a single number, giving you a clear picture of how your microbiome stacks up.)
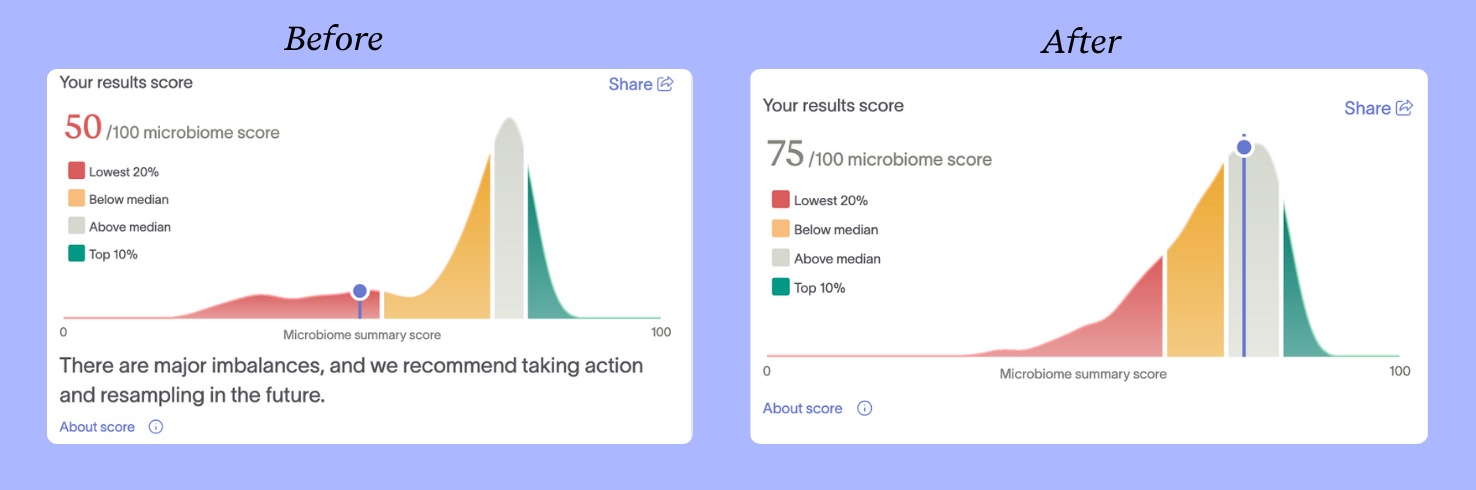
A Baby Gut Test advocate is born
"Myles is now the happiest one-and-a-half-year-old in the world," says Torie. With no food off-limits now, Myles can have everything, including whole milk, tomatoes, cupcakes, and everything that used to make him sick.
After such a heartbreaking year, Torie is eager to share her story with other parents facing similar struggles. She’s passionate about letting them know what she learned about the link between antibiotic use and gut dysbiosis—imbalances which can have negative long-term health effects [5].
"I firmly believe so strongly that I tell everybody about Tiny Health. Every single mom friend knows exactly what fixed him, and they know I tried everything under the sun."
Looking through photos from Myles' first year, Torie recalled the smiles and good times they shared. However, tears clouded those memories. She said, “I remember my mom saying, ‘He wants to be happy; he just doesn't feel good.’”
“I'm so glad I listened to my inner voice over everyone telling me to give up,” Torie said. “It still blows my mind sometimes. We'll be playing with his toys or eating dinner, and he'll get up and run around the house, and I say to my husband, 'Honey, look how happy he is. Remember how sad he was a year ago? How did we get through that?'"
Now approaching the birth of her second child, Torie is more than prepared. She knows Tiny Health has her back if her newest addition has any tummy troubles.
Are you navigating a similar journey with your little one? Tiny+ Baby Membership is designed to help you uncover underlying imbalances that might be contributing to your child's chronic conditions. With 1-on-1 consultations with microbiome specialists, we're here to provide you with personalized guidance, every step of the way.






