Lila’s* son, Rowan, seemed to be off to a great start. He was sleeping through the night, eating well, and meeting his milestones. Born via C-section, he appeared healthy in every way.
That changed at three months, when Rowan began having bloody, mucus-filled stools up to 12 times a day. Over the next few months, Lila visited multiple pediatricians, who suspected a dairy or soy allergy. She cut both from her diet while breastfeeding, but the bleeding persisted.
Reflecting on that challenging time, Lila shared how exhausting those months were, the mom guilt, and the huge relief she felt when she finally understood exactly what was going on. The steps she took to get Rowan’s gut back on track turned out to be surprisingly simple.
* To respect the privacy of this Tiny Health family, we've changed names and used a photo representation. The following case study, including their Baby Gut Health Test results and screenshots, are 100% authentic to their experience with us.
The search for answers
Cutting out dairy and soy while breastfeeding seemed practical, but nothing improved.
One pediatrician hinted she wasn’t trying hard enough. Another pushed for a full elimination diet to determine what was causing the bleeding. By this point, Lila was about 10 pounds below her pre-pregnancy weight, and her milk supply dipped. Stressed and anxious that something in her diet was hurting Rowan, she became vigilant, preparing every meal at home and double-checking every label. Still, doctors insisted it was something in her breastmilk.
“I felt like a failure…even though I was cooking all of my meals and being religious about not consuming any dairy or soy.”
She was so determined to eliminate every possible trigger that she and her husband stopped sharing meals entirely.
The relentless diaper changes, the uncertainty, and feeling unheard took a toll on Lila.
“Emotionally, I felt immense ‘mom guilt’ every time I saw blood in my son’s stool.”
On a particularly tough day, Lila had to cancel a work meeting to take her son back to the pediatrician after a larger-than-usual amount of blood in his diaper. Hours later, a check-in with her manager would change everything: her boss recommended Tiny Health.
That night, Lila ordered a baby gut health test, hoping, finally, for some answers.
Out of the dark and into the data
Rowan’s results came back, confirming what Lila had sensed all along: his digestive system was in distress. His Microbiome Summary Score was 38 out of 100, signaling major imbalances.
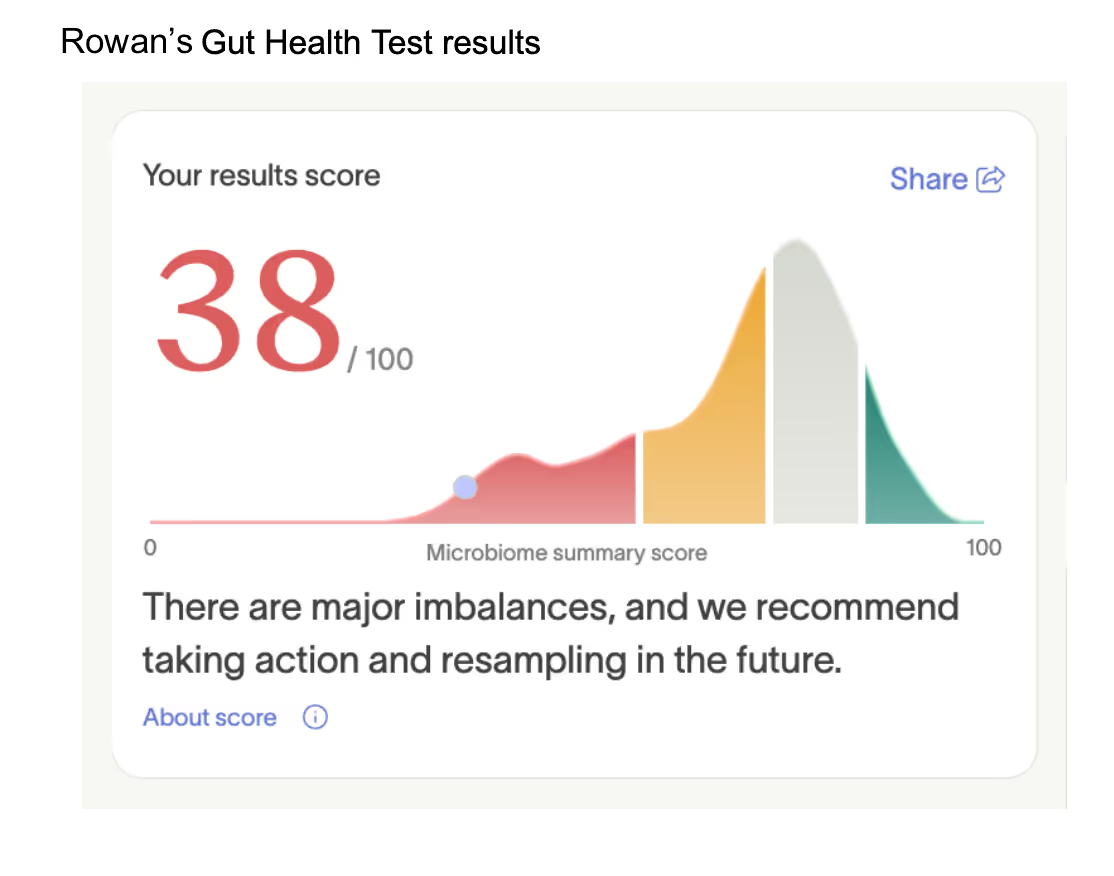
“To be honest, I cried when I opened the report. Seeing how low on the scale my son’s gut health was made me feel awful. But I knew there was something wrong, and I was just grateful to have answers.”
One of the most concerning findings: Rowan had 0% beneficial Bifidobacterium, which should dominate an infant’s gut during the first year of life [1]. These bacteria support healthy digestion, train the immune system, and strengthen the gut barrier [2]. Having high levels of Bifidobacterium bacteria helps to create an environment in the gut where the growth of disruptive microbes is inhibited [1].
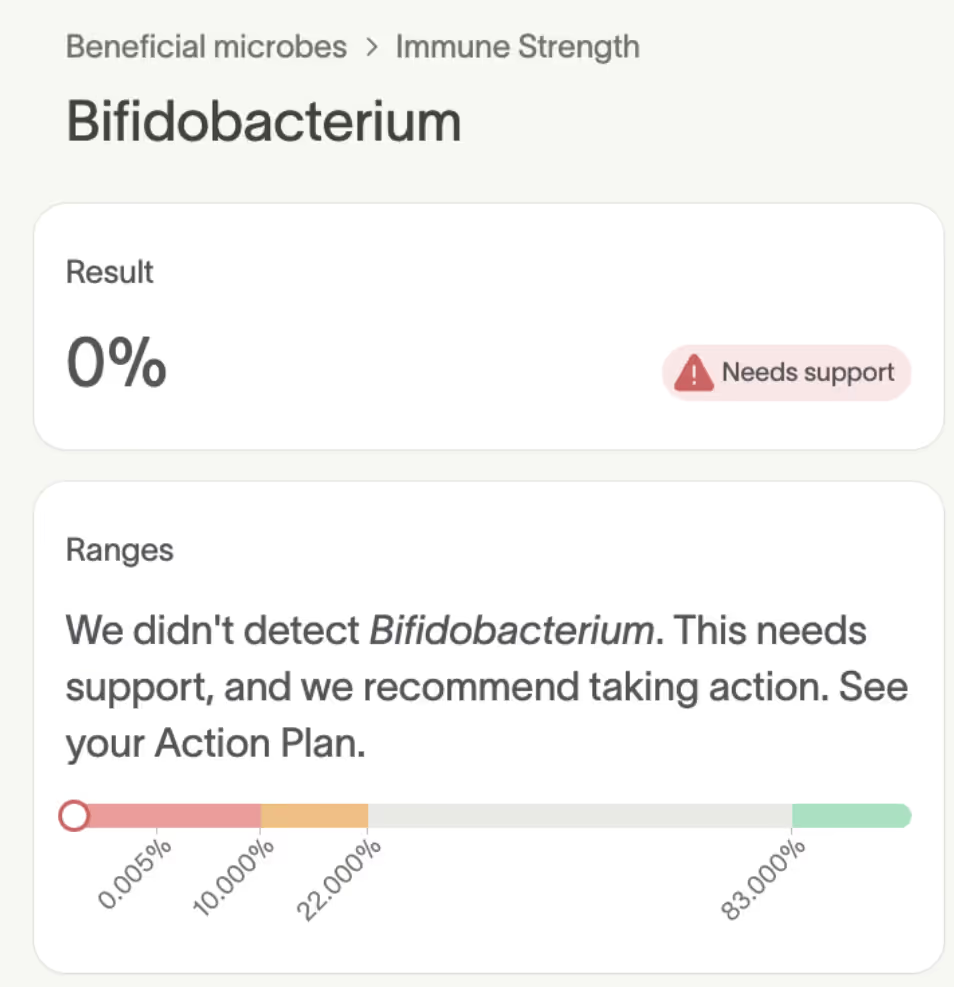
Rowan also had 0% HMO-digesting Bifidobacterium, the specific strains that help break down the complex sugars in breastmilk.
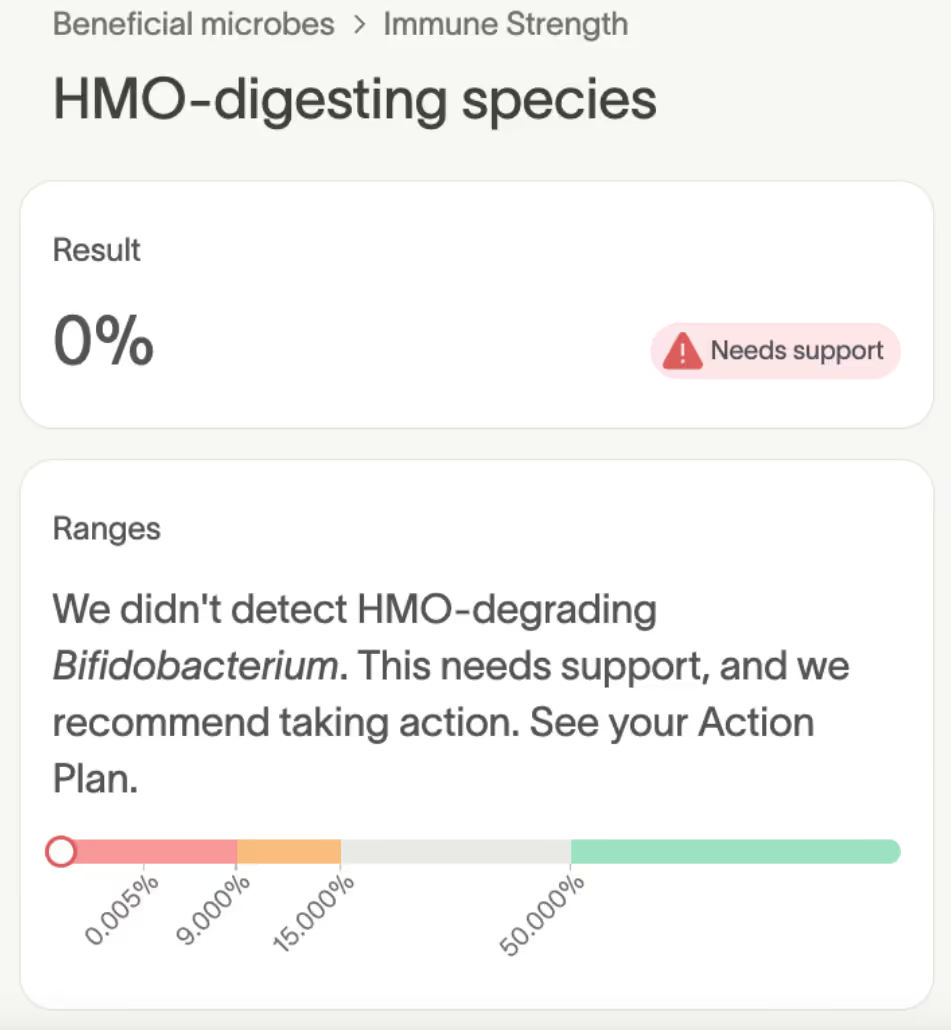
HMO-digesting Bifidobacterium should be well-established for a six-month-old. Their absence confirmed what his broader results had already shown: his gut was missing important microbes needed to support healthy immune development.
Rowan's results also showed a high C-section signature, a microbial pattern often seen in babies born by cesarean delivery. Research shows that during birth, babies are seeded with mom's microbes [1]. Cesarean delivery skips the usual transfer of helpful bacteria from mom to baby, which can delay the growth of good microbes and lead to lower diversity in the baby’s gut in early life [1]. This signature explains why babies, like Rowan, need extra support to establish beneficial bacteria for their short and long-term health.

Rowan’s gut profile showed Metrics related to conditions: eczema, colic, and cow’s milk protein allergy (CMPA). These correlations suggest imbalances might be contributing to his symptoms, but they are not a diagnosis.

Rowan’s Microbiome breakdown showed that 99% of his gut bacteria were classified as unfriendly.
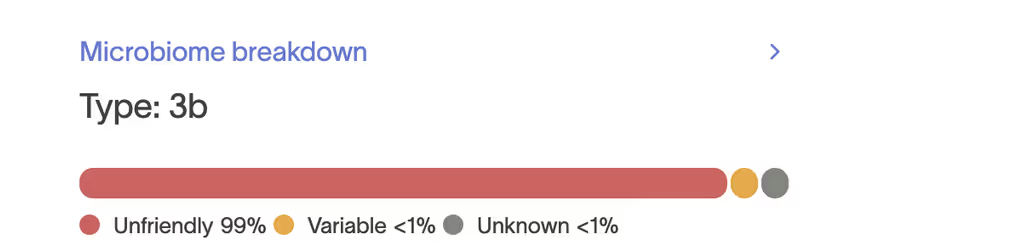
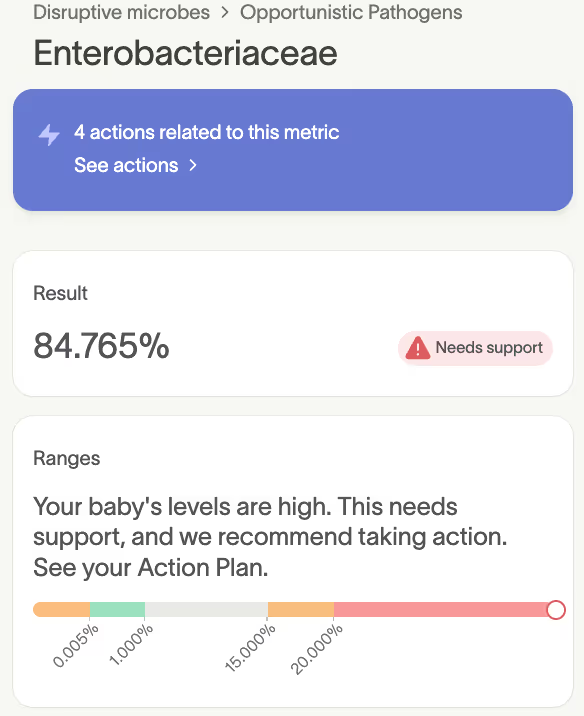
84.8% of Rowan’s gut microbiome was made up of Enterobacteriaceae, a family of bacteria that includes opportunistic pathogens like Klebsiella, Citrobacter, and Enterobacter.
Enterobacteriaceae microbes aren’t inherently dangerous, but when they show up in high levels in the absence of protective bacteria like Bifidobacterium, they can contribute to inflammation [3].
A step-by-step plan
After months of stress, guilt, and guessing, Lila finally had something solid: test results with a detailed Action Plan. And the tools to rebalance Rowan’s gut.
Over a dozen of Rowan’s microbiome metrics were flagged as ‘Needs Support’. But three recommendations stood out as the most impactful.

Since Rowan completely lacked the Bifidobacterium species that digest HMOs, continuing to provide breastmilk — even in small amounts — was crucial to support the growth of these beneficial bacteria. And when supplementing with formula, using one with added HMOs offers similar benefits for a baby’s gut.
To support Rowan's gut and brain development and Lila's postpartum recovery, omega-3 supplements were another targeted recommendation. Whether including 2–3 servings of fatty fish each week in her diet or adding a high-quality fish oil supplement, this step helped nourish both mom and baby.
Rowan’s Action Plan also suggested limiting antibiotics, getting outside regularly, and increasing contact with animals.
During her consultation with Tiny Health's microbiome specialist Kathleen Comerford, Lila found comfort in how Kathleen explained Rowan's results. Kathleen went over how to introduce the Bifidobacterium probiotic, how to time it with feedings, and how long to stay on it.
"Kathleen was great. She was efficient, sensitive, informative, and solution-oriented!”
Lila started Rowan's on the probiotic immediately and began taking omega-3s herself.
Things turned around fast
The morning after the first dose of the probiotic, things shifted.
“The bleeding and mucus were gone. His poops were normal, and he was down to just one or two diapers a day. This happened within a day of him taking those probiotics. I cried the first time I changed his diaper, and there was no blood.”
Since his Bifidobacterium imbalances were addressed, Rowan has stayed symptom-free. Even after reintroducing the foods Lila had been told to avoid, her son is thriving.
Lila didn’t expect such fast results or the seismic relief when the stress and guilt disappeared. No more analyzing every diaper like a detective.
Like many parents who faced similar challenges with their little ones, Lila felt frustrated about how long it took to find answers.
“There is a part of me that is angry about the false diagnosis, which in turn caused my son to bleed for months longer than he should have, and for me to blame myself."
Our tests don’t replace medical care, so Lila did the right thing by first ruling out any serious causes of bleeding with Rowan’s pediatricians.
While she wishes she had known about the Baby Gut Health Test sooner, what matters most is the peace it brought her family and the confidence that came with finally being able to support her son.
When she hears of another baby struggling, she’s quick to share the results that brought clarity.
.avif)






