Red flags, “Maybe they’ll just grow out of it,” and a trip to the ER. These are a few things no parent wants to experience—yet Chloe and her husband, Luke, found themselves in unfamiliar territory as both their kids suffered from eczema. The endless itching, sleepless nights, and barely working creams left them exhausted and desperate for answers.
Eczema is common in kids, and most treatments focus on calming the skin. But a functional approach looks deeper, asking what’s causing this*. For some little ones, the answer is in the gut. If the trillions of microbes living there are out of balance, skin issues like eczema can flare up [1].
In our exchange with Chloe, she shared her experience managing her children’s eczema journey—complete with scary moments, frustration, and, eventually, a breakthrough in a place she never expected.
When things don’t go as planned
For Chloe and her husband, Luke, life is a juggling act—work, daycare drop-offs, and the typical chaos of raising little ones. The couple always wanted two kids close in age. So, they went for the two-under-two route, and life has been nonstop since welcoming Carmen, now 2.5 years old, and Charlie, 16 months.
The family's journey with eczema began in a roundabout way when Carmen was just four weeks old. When Chloe saw blood in Carmen's stool, alarm bells went off. What followed was weeks of allergy testing and dietary changes, eventually leading to a cow's milk protein sensitivity diagnosis.
At around two months old, Carmen developed red, dry patches on her skin—first on her cheeks and chin, then spreading to her thighs and forearms. The condition only worsened as she grew older.

Chloe’s second child, Charlie, didn’t have milk protein issues, but when it came to his skin, he followed in his sister’s footsteps. He developed even more severe dry patches on his arms, torso, and behind his knees.
Doctors told Chloe and Luke that their kids might grow out of it—or it would just be something they’d have to manage until they got older, with creams, cool baths, hydrocortisone for flare-ups, and avoiding trigger foods like dairy.
Managing eczema became part of the family’s nightly routine: baths in lukewarm water (which the kids hated, especially in the winter), followed by slathering them in Aquaphor before getting them into pajamas. Even with those cautionary steps, Carmen and Charlie still had flare-ups.
Searching for answers through late-night scrolls
Chloe explained, “To say this was challenging and stressful would be an understatement, and I can’t really begin to articulate exactly how much this affected not only our family but also my mental health as a new mom of two under two.”
Chloe spent hours researching on the internet, scouring discussion boards, and trying to find solutions for her babies. “It was heartbreaking to see them uncomfortable, and at times, as they got older, they would scratch until they bled,” Chloe said.
Chloe shared that as a parent, few things are more heartbreaking than seeing your child suffer—especially when it feels like you’ve tried everything and nothing seems to work.
“It was incredibly hard, and looking back on that time now, I truly wish I had known about (and understood more) what Tiny Health could do,” Chloe continued.
Their trip to the ER was a turning point
The couple hit a breaking point when Charlie was around seven months old, struggling through a terrible flare-up while also fighting off a virus. Charlie’s immune system went into overdrive—he started wheezing and broke out in full-body hives. They rushed him to a children’s hospital, where he received a shot of epinephrine. This experience made them realize they needed to search deeper for answers.
.avif)
Chloe had seen ads for Tiny Health on Instagram many times before she decided to do something. “I tended to think it was just Instagram trying to influence me into another product that may or may not work.”
But in a moment of desperation, Chloe decided to give it a try. “I just remember seeing eczema on his little forearms looking so painful one night in the bath,” Chloe recalls. “I pulled out my phone right there and bought a Tiny Health kit for both my kids. I figured, what can it hurt? I was at my wit’s end.”
Charlie’s test results
Tiny Health’s baby gut microbiome tests revealed that Charlie had imbalances in his gut, potentially contributing to his skin conditions and impacting his overall immune health.
One of the areas that was flagged as needing support was Charlie’s gut maturation. His microbiome was too mature for a baby his age. Ideally, a baby's gut microbiome maturation stays low before four months and reaches adult-like maturity by 3–5 years old. A gut that matures too quickly may miss critical developmental windows for immune training and protection.
To course correct, Chloe followed her Action Plan recommendation: feeding Bifidobacterium what they love, human milk oligosaccharides (HMOs), special sugars found in breastmilk.
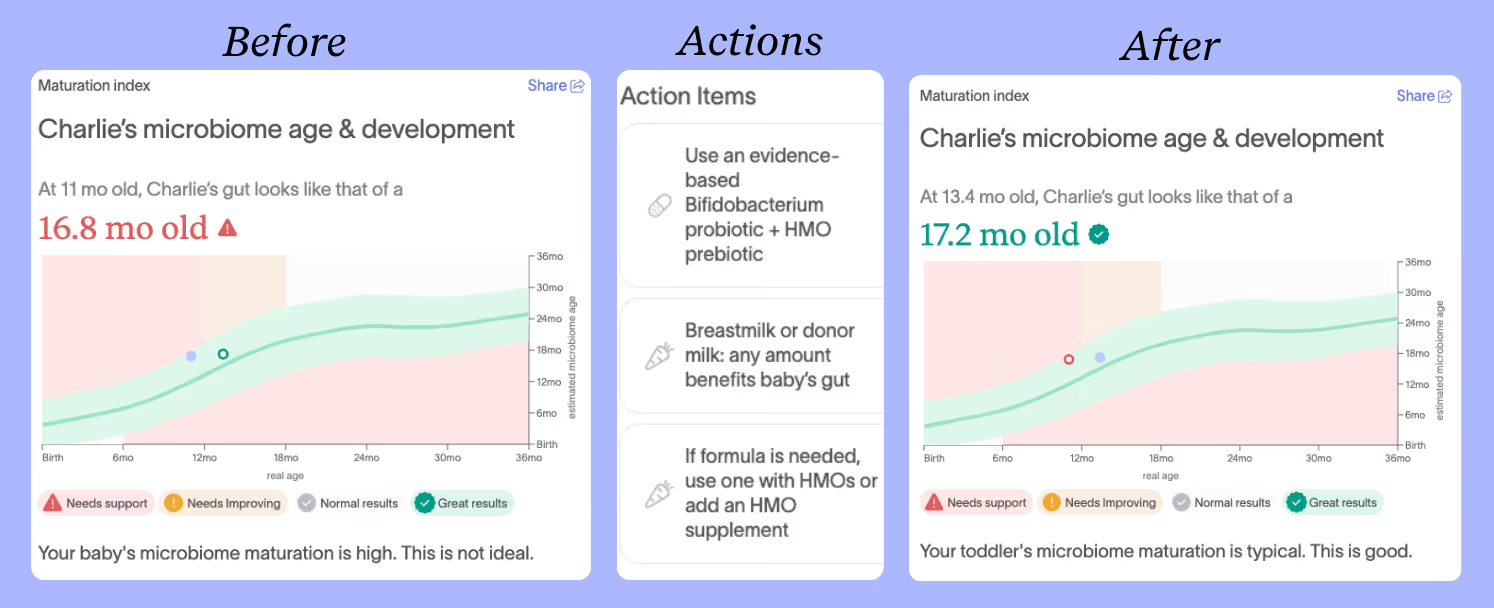
Charlie's test also showed HMO-digesting species at just 4.74%. This meant Charlie's gut was missing the key bacteria needed to fully unlock the benefits of breastmilk.
Bifidobacterium is essential to a baby’s gut health because it breaks down HMOs, producing short-chain fatty acids that support immune development, nutrient absorption, and much more.
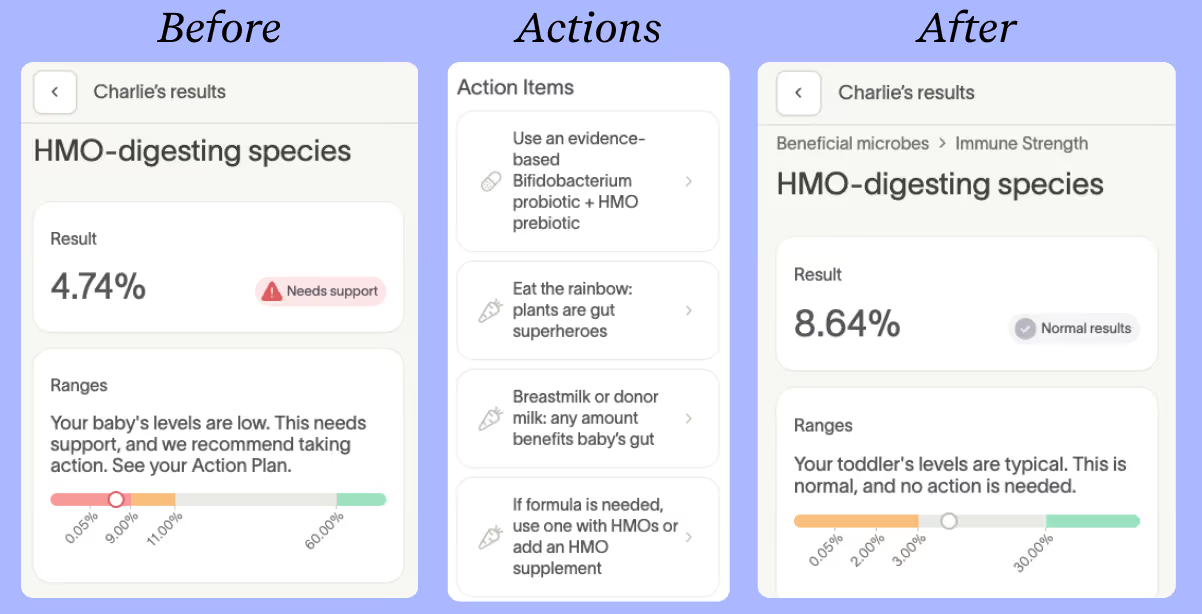
Chloe paired a Bifidobacterium probiotic with an HMO and added plant diversity to Charlie's diet to bring his score up.
Charlie's symptoms improved almost immediately. "It was so fast that my husband and I were in disbelief. Within two weeks, his eczema patches reduced by almost 80%, and within a month, they were gone completely."
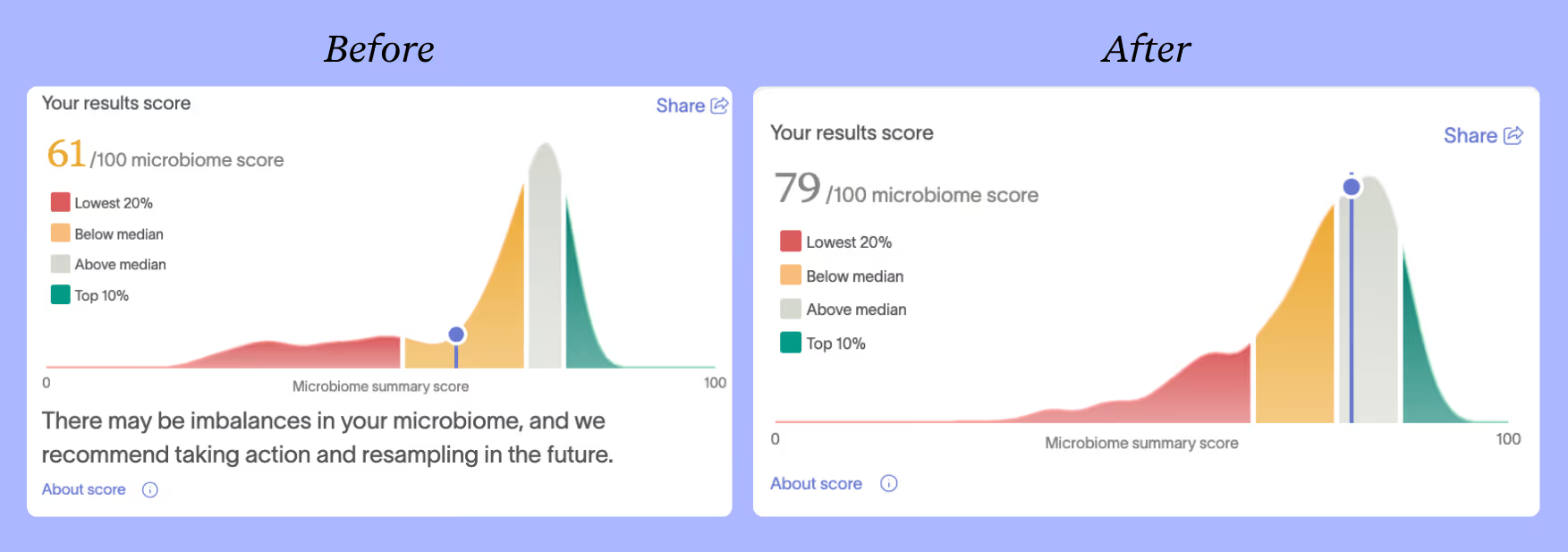
His retest confirmed the transformation. Charlie's Microbiome Summary Score jumped from 61 to 79.
Carmen’s test results
Carmen's test results revealed a Shannon diversity score of 4.8, flagged as needs improving, and an eczema signature. This borderline low diversity means her gut had less variety of bacteria species than ideal. Some bacteria levels were slightly above or below the expected range for her age. Low diversity and certain strains of disruptive bacteria are often linked to an increased microbiome risk of atopic march conditions [2].
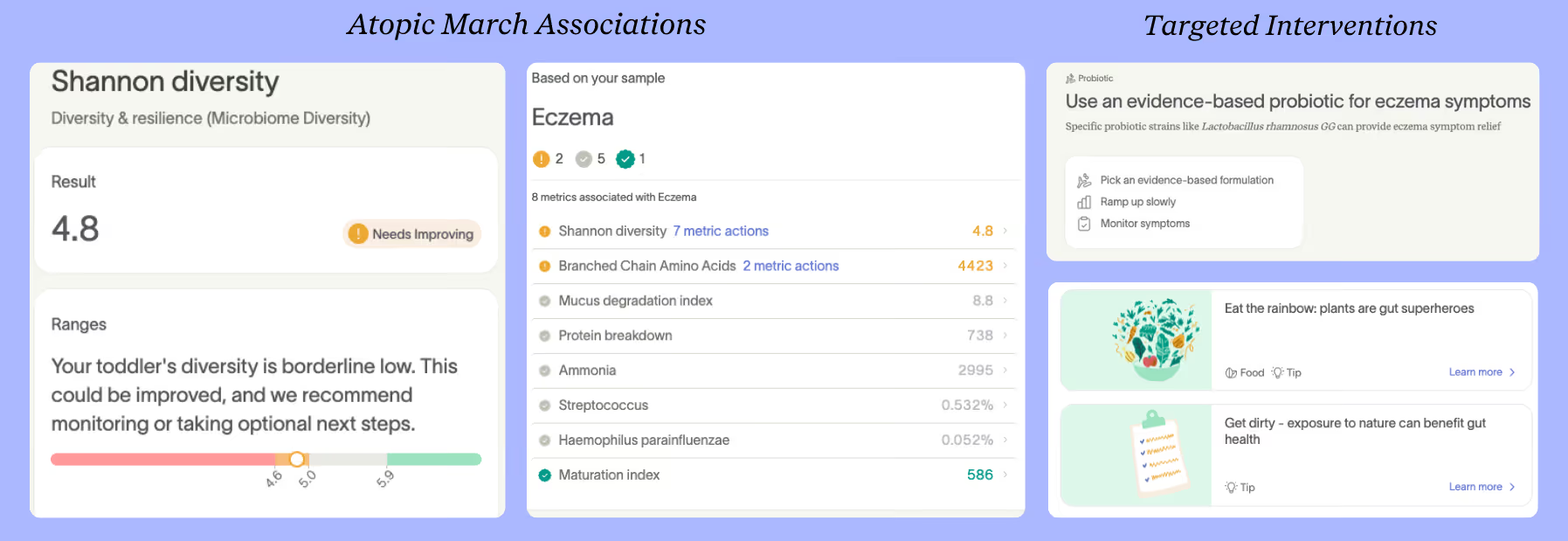
Carmen's Action Plan included targeted interventions: an evidence-based probiotic containing Lactobacillus rhamnosus GG to help with eczema symptoms, eating the rainbow to boost gut diversity through plant foods, and outdoor play. Chloe noted that the targeted probiotics in the Action Plan put her at ease because they were backed by science.
Carmen’s outcome was just as positive. Neither of Chloe's children have had any flare-ups or even a single eczema patch since. “I’ve also noticed that both kids seem to get over their illnesses much quicker," Chloe said.
.avif)
One-on-one support made all the difference
Chloe found the session with Tiny Health’s microbiome specialists especially helpful: “It was one of the best parts of the entire experience. I got someone knowledgeable… and they walked me through each part of the results report and the corresponding action plan. I had hesitated to do the coaching at first, but I am so glad I did it. It was maybe one of the most valuable and insightful experiences I’ve ever had.”
One of the things they touched on was food and lifestyle recommendations in the Action Plan. Chloe added more fermented foods to the kids' meals and learned how exposure to various microorganisms, including those from pets, farm animals, and soil, benefits gut health. She brought them outdoors almost every day and even ditched the hand sanitizer, leaning into more natural ways to support her kids' immune health.
For Chloe, the combination of expert guidance and actionable recommendations gave her the confidence to make changes that work for the whole family.
Celebrating the wins
“I finally had answers I couldn’t find anywhere else, either from the internet, discussion boards or even in talking to our pediatrician.”
Once filled with short, tepid baths and oily ointments, their nightly routine has transformed into a fun, joyful time with bubble baths and bedtime stories, Chloe shared.
“I really can’t emphasize the positive impact this has had on us in a totally unexpected way,” Chloe added.
The biggest win? Chloe’s kids can now just enjoy being kids, free from the discomfort of eczema or the anxiety of food sensitivities. She hopes these early interventions continue to support their immune systems and overall wellness, allowing them to thrive in everything they do.
Answers from the inside out
As Chloe and Luke learned firsthand, gut imbalances can greatly impact eczema. When they moved beyond skin treatments and focused on the root cause—gut imbalances—they finally found relief for Carmen and Charlie. Tiny Health’s Baby Gut Health Test gave them the insights they needed. And with personalized recommendations, they saw lasting improvements in their kids' gut, skin, and general health.
If you’re dealing with eczema in your family and looking for answers beyond the surface, explore how gut health could be the missing link. Find out if your baby's gut microbes might be at the root of their eczema. Tiny Health’s Eczema Gut Rebalance membership provides valuable, science-backed insights into your child's unique gut microbiome.
* Tiny Health's clinical trial, Infant Restore, found that a 6-month intervention program reduced the odds of eczema in C-section babies by 83%. If your little one is just starting out, supporting their gut microbiome early on may help protect against eczema and set the foundation for long-term health. Download our Infant Restore White Paper to learn more.








