Your fertility journey starts months before ovulation. Egg quality depends on hormones, metabolism, inflammation, and your microbiome. Both the gut and vaginal microbiomes play key roles in reproductive health, from egg development to implantation. Learn how diet and lifestyle changes can support your microbiome and naturally improve fertility.
How to Boost Fertility Naturally by Supporting Your Microbiome

Summary
When we talk about fertility, we often focus on the “big events”: ovulation, fertilization, and implantation. But long before those moments occur, your body is preparing for pregnancy through a complex network of systems, including your hormones, immune system, metabolism, and microbiome.
If you're wondering how to improve fertility naturally, this process starts months before ovulation and depends on more than just hormones.
Two microbial ecosystems play an especially important role: the gut microbiome and fertility are closely connected, as are the vaginal microbiome and fertility outcomes.
Fertility starts months before ovulation
Many people think fertility begins when an egg is released during ovulation. In reality, the process starts much earlier.
Eggs take about 3–4 months to fully mature before ovulation. During this time, they are highly sensitive to the environment surrounding them.
For eggs to develop normally, they need:
- Healthy mitochondria (the tiny energy factories inside the cell that power early embryo development)
- Balanced hormones
- Low levels of inflammation and oxidative stress [1], [2]
If the egg environment becomes disrupted, fertilization and embryo development may struggle, even if ovulation occurs normally.
Egg quality naturally declines as you age
One of the strongest factors affecting fertility is age. Women are born with all the eggs they will ever have, and both the number and quality of those eggs gradually decline over time.
At birth, the ovaries contain millions of immature eggs. By puberty, around 300,000–500,000 remain, and that pool continues shrinking with every cycle. By age 30, about 90% of the original egg reserve has already been lost, and by age 40, only a small fraction remains [3].
Egg quality also changes with age. As eggs get older, they are more likely to develop chromosomal errors during cell division, which can make conception harder and increase the risk of miscarriage [4].
Egg quality refers to how healthy an egg is and how likely it is to develop into a viable embryo. It is influenced by age, inflammation, mitochondrial function, and the environment in which the egg matures.
But age is not the only factor that influences fertility.
Two women of the same age can have very different fertility outcomes, suggesting that the environment surrounding the eggs also matters.
Your eggs need the right environment to thrive
Think of your developing egg like a seed.
The soil surrounding it is the follicular fluid inside the ovary. This environment is shaped by signals from the ovary and the body. When it becomes inflamed or metabolically stressed, the egg may not develop optimally [5], [6].
Researchers have found that aging ovaries often develop fibrosis, a type of stiff scar-like tissue that increases inflammation and makes the ovarian environment less supportive for egg development [7].
Egg cells are also extremely sensitive to oxidative stress, which can damage their mitochondria, the energy systems required for early embryo growth [8].
This is where systemic factors such as diet, metabolic health, and the gut microbiome begin to influence fertility and egg quality.
How your gut microbiome influences fertility and egg quality
The gut microbiome plays a key role in fertility by regulating many processes that influence reproductive health, including:
- Inflammation
- Estrogen metabolism
- Blood sugar regulation
- Immune signaling [9]
If the gut microbiome becomes imbalanced, inflammatory molecules can leak into the bloodstream. Animal studies show that this systemic inflammation can reach the ovaries and potentially damage the delicate mitochondria of developing eggs [5], [6].
Because diet strongly shapes the gut microbiome [10], nutrition during the months leading up to conception may influence egg quality [11]- [13].
How your vaginal microbiome can affect your chances of getting pregnant
While the gut microbiome influences egg development, the vaginal microbiome plays a key role in fertility and implantation.
A healthy vaginal microbiome is typically dominated by Lactobacillus bacterial species, which help maintain an acidic environment that protects the reproductive tract from disruptive microbes [14].
A balanced vaginal microbiome is increasingly recognized as an important factor in fertility and in vitro fertilization (IVF) success. Studies have found that women with Lactobacillus-dominant vaginal microbiomes tend to have higher IVF success rates, while microbial imbalances are associated with lower implantation rates and higher pregnancy loss [15]-[17].
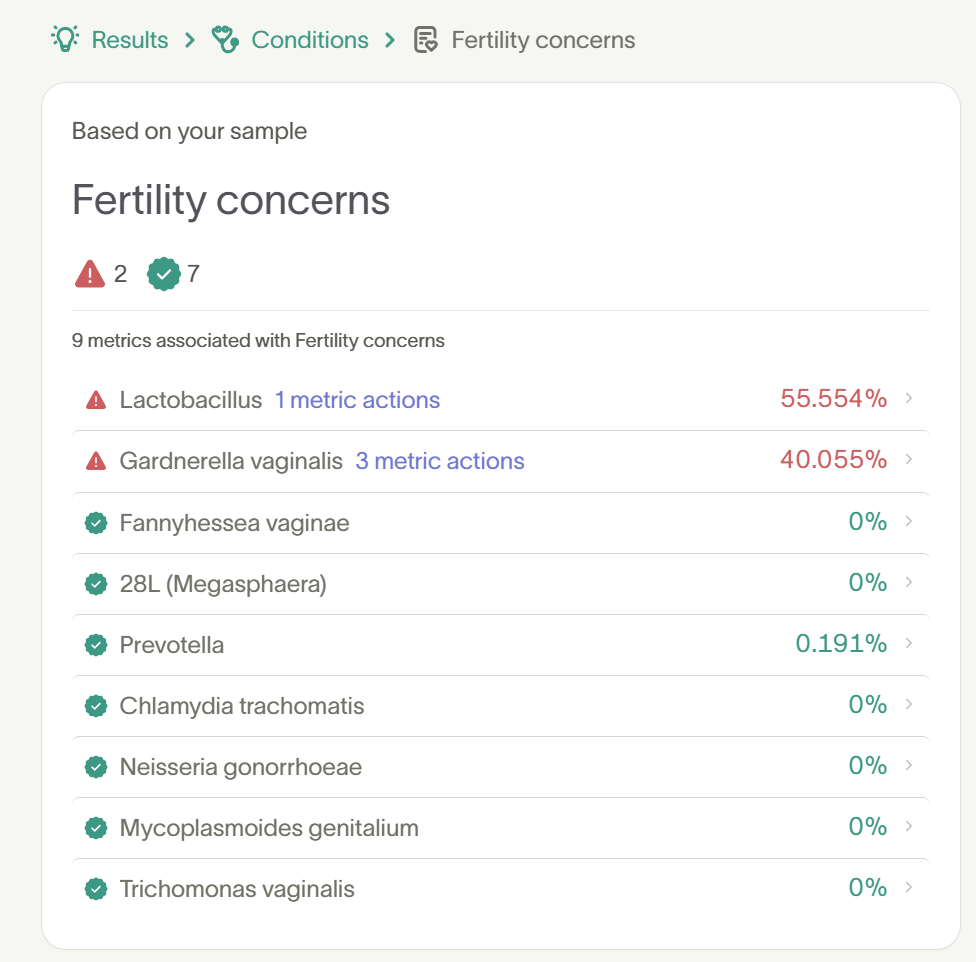
For this reason, Tiny Health vaginal microbiome reports highlight microbial patterns that research has linked with fertility outcomes. You can find the metrics associated with fertility under Metrics related to conditions > Fertility concerns.
How your diet shapes your egg quality
Research from animal and human studies suggests that diet can influence fertility through its effects on metabolism and the microbiome [11]-[13].
For example:
- High-fat diets and obesity have been shown to reduce egg quality in animal studies [11], [12]
- Omega-3 fatty acids can improve egg quality and may extend reproductive lifespan [13], [18]
- Diets rich in folate have been associated with better outcomes in fertility treatments [19]
Diet can also influence the environment of the uterus. For example, research shows that following a Mediterranean-style diet can change the chemical environment of the uterus during the window when implantation occurs, which may affect fertility outcomes [20].
The vaginal microbiome can also respond to diet. Women following an ‘unhealthy’ diet (high in sweets and desserts, refined grains, sweet drinks, solid oils) are at higher risk of developing bacterial vaginosis [21].
Many of these effects are mediated by the gut microbiome, which helps transform nutrients into molecules that regulate inflammation and hormonal balance.
4 areas that affect your fertility and how to support them
Fertility is not controlled by a single organ, but by the interaction between hormones, metabolism, the immune system, and the microbiome.
Here are some ways to support your gut and vaginal microbiomes and the environment in which your eggs mature:
1. Support your gut (and vaginal) microbiome
- Eat a fiber-rich diet with vegetables, legumes, whole grains, and fruits to feed beneficial gut bacteria.
- Include fermented foods such as yogurt, kefir, kimchi, or sauerkraut to introduce beneficial microbes.
- Limit ultra-processed foods and excessive added sugar, which can promote inflammation and metabolic imbalance.
2. Support metabolic health
- Aim for stable blood sugar by combining protein, healthy fats, and fiber at meals.
- Prioritize regular physical activity, which improves insulin sensitivity and reduces inflammation.
- Maintain adequate sleep, since poor sleep can disrupt metabolic and reproductive hormones.
3. Reduce inflammation and oxidative stress
- Include foods rich in antioxidants, such as berries, leafy greens, nuts, and olive oil.
- Ensure adequate intake of key nutrients linked to reproductive health, such as folate and omega-3 fatty acids.
- Avoid smoking and limit alcohol, which can increase oxidative stress and may affect egg quality.
4. Support a healthy vaginal microbiome
- Avoid unnecessary vaginal products such as douches or fragranced washes that disrupt natural microbial balance.
- Choose breathable cotton underwear and avoid prolonged moisture, which can promote microbial imbalance.
- Seek treatment for recurrent infections or symptoms that may indicate vaginal dysbiosis.
This approach may be especially helpful for people trying to conceive naturally or preparing for fertility treatments such as IVF.
Fertility FAQ
How do you know if you're infertile?
The best first step is to talk to a fertility specialist, especially if you've been trying to conceive for 12 months without success (or 6 months if you're over 35).
Some signs worth discussing with your practitioner sooner rather than later include irregular or absent periods, very painful cycles, recurrent miscarriages, or known conditions like PCOS or endometriosis.
Many people with fertility challenges don't have obvious symptoms at all — which is why working with a specialist matters.
Can you improve egg quality naturally?
While you can’t change your age or the number of eggs you have, you can support the environment in which eggs mature. Diet, metabolic health, inflammation, and your microbiome may all influence egg quality.
How does the gut microbiome affect fertility?
The gut microbiome helps regulate hormones, inflammation, and metabolism, all of which play a role in egg development and reproductive health.
Does the vaginal microbiome affect pregnancy?
Yes. A Lactobacillus-dominant vaginal microbiome is associated with better reproductive outcomes, including higher implantation and IVF success rates.
What’s the best way to balance female hormones naturally?
Your gut microbiome plays a direct role in hormone balance by helping metabolize estrogen and regulating inflammation [Mora 2025]. Eating a fiber-rich diet, including fermented foods, keeping blood sugar stable, staying active, and getting consistent sleep all support the systems that keep your hormones in check.
Can ovarian cyst cause infertility?
It depends on the type. Functional cysts, which form during a normal menstrual cycle, usually resolve on their own and don't affect fertility. Cysts related to conditions like PCOS or endometriosis are more likely to interfere with ovulation and egg development. If you're concerned, talk to your practitioner. They can help determine what type of cyst you're dealing with and whether it needs treatment.
Can birth control cause you to be infertile?
Highly unlikely. A systematic review of over 14,000 women found that contraceptive use, regardless of type or duration, did not negatively affect the ability to conceive after stopping [22]. Most methods allow fertility to return within a few cycles, though the timeline varies. Injectable contraceptives like Depo-Provera may take up to 18 months.
If you've been trying for 12 months without success (or 6 months if you're over 35), talk to your practitioner to rule out other factors.

Baby’s health starts with you
References
References
[1] X. Zhang, L. Zhang, and W. Xiang, “The impact of mitochondrial dysfunction on ovarian aging,” J. Transl. Med., vol. 23, no. 1, p. 211, Feb. 2025.
[2] E. Moustakli et al., “Oxidative stress and the NLRP3 inflammasome: Focus on female fertility and reproductive health,” Cells, vol. 14, no. 1, p. 36, Jan. 2025.
[3] W. H. B. Wallace and T. W. Kelsey, “Human ovarian reserve from conception to the menopause,” PLoS One, vol. 5, no. 1, p. e8772, Jan. 2010.
[4] W. Huang, X. Li, H. Yang, and H. Huang, “The impact of maternal age on aneuploidy in oocytes: Reproductive consequences, molecular mechanisms, and future directions,” Ageing Res. Rev., vol. 97, no. 102292, p. 102292, Jun. 2024.
[5] Z. Fan et al., “Intestinal flora changes induced by a high-fat diet promote activation of primordial follicles through macrophage infiltration and inflammatory factor secretion in mouse ovaries,” Int. J. Mol. Sci., vol. 23, no. 9, p. 4797, Apr. 2022.
[6] J. Wen et al., “High-fat diet-induced L-saccharopine accumulation inhibits estradiol synthesis and damages oocyte quality by disturbing mitochondrial homeostasis,” Gut Microbes, vol. 16, no. 1, p. 2412381, Jan. 2024.
[7] E. Ouni et al., “Spatiotemporal changes in mechanical matrisome components of the human ovary from prepuberty to menopause,” Hum. Reprod., vol. 35, no. 6, pp. 1391–1410, Jun. 2020.
[8] Y. Xie et al., “Oocyte-specific deletion of Gsα induces oxidative stress and deteriorates oocyte quality in mice,” Exp. Cell Res., vol. 370, no. 2, pp. 579–590, Sep. 2018.
[9] P. Escorcia Mora, D. Valbuena, and A. Diez-Juan, “The role of the gut Microbiota in female reproductive and gynecological health: Insights into endometrial signaling pathways,” Life (Basel), vol. 15, no. 5, p. 762, May 2025.
[10] G. Fackelmann et al., “Gut microbiome signatures of vegan, vegetarian and omnivore diets and associated health outcomes across 21,561 individuals,” Nat. Microbiol., vol. 10, no. 1, pp. 41–52, Jan. 2025.
[11] R. L. Robker, “Evidence that obesity alters the quality of oocytes and embryos,” Pathophysiology, vol. 15, no. 2, pp. 115–121, Aug. 2008.
[12] M. Sohrabi, A. M. Roushandeh, Z. Alizadeh, A. Vahidinia, M. Vahabian, and M. Hosseini, “Effect of a high fat diet on ovary morphology, in vitro development, in vitro fertilisation rate and oocyte quality in mice,” Singapore Med. J., vol. 56, no. 10, pp. 573–579, Oct. 2015.
[13] D. Nehra et al., “Prolonging the female reproductive lifespan and improving egg quality with dietary omega-3 fatty acids,” Aging Cell, vol. 11, no. 6, pp. 1046–1054, Dec. 2012.
[14] J. Ravel et al., “Vaginal microbiome of reproductive-age women,” Proc Natl Acad Sci U S A, vol. 108 Suppl 1, no. Suppl 1, pp. 4680–4687, Mar. 2011.
[15] G. Campisciano et al., “Subclinical alteration of the cervical-vaginal microbiome in women with idiopathic infertility,” J Cell Physiol, vol. 232, no. 7, pp. 1681–1688, Jul. 2017.
[16] Y. Kong et al., “The Disordered Vaginal Microbiota Is a Potential Indicator for a Higher Failure of in vitro Fertilization,” Front Med (Lausanne), vol. 7, p. 217, 2020.
[17] R. Koedooder et al., “The vaginal microbiome as a predictor for outcome of in vitro fertilization with or without intracytoplasmic sperm injection: a prospective study,” Hum Reprod, vol. 34, no. 6, pp. 1042–1054, Jun. 2019.
[18] A. J. Gaskins and J. E. Chavarro, “Diet and fertility: a review,” Am. J. Obstet. Gynecol., vol. 218, no. 4, pp. 379–389, Apr. 2018.
[19] H. Chen, S. Wang, M. Song, D. Yang, and H. Li, “Oocyte and dietary supplements: a mini review,” Front. Cell Dev. Biol., vol. 13, p. 1619758, Jun. 2025.
[20] N. M. Molina et al., “Endometrial whole metabolome profile at the receptive phase: influence of Mediterranean Diet and infertility,” Front. Endocrinol. (Lausanne), vol. 14, p. 1120988, Apr. 2023.
[21] M. Noormohammadi, G. Eslamian, S. N. Kazemi, and B. Rashidkhani, “Association between dietary patterns and bacterial vaginosis: a case-control study,” Sci. Rep., vol. 12, no. 1, p. 12199, Jul. 2022.
[22] T. Girum and A. Wasie, “Return of fertility after discontinuation of contraception: a systematic review and meta-analysis,” Contracept. Reprod. Med., vol. 3, no. 1, p. 9, Jul. 2018.